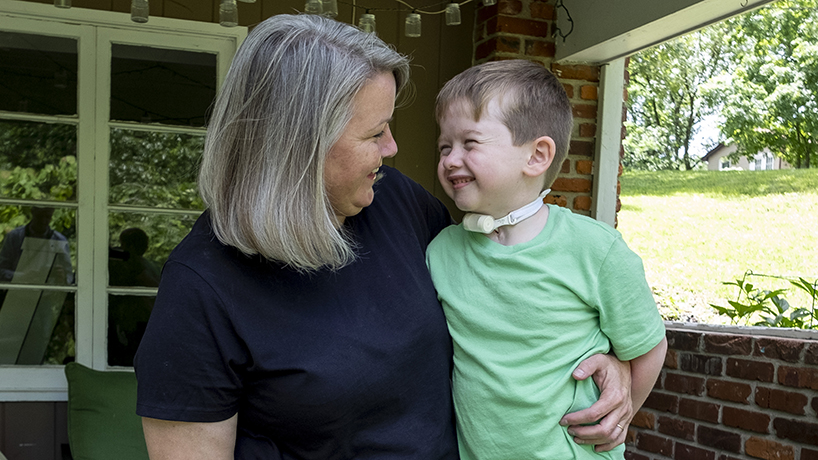
Alumna Kim Rankin used skills and knowledge gained at UMSL to inform the care and education of her adopted son, Nathaniel, who was born with a trachea measuring 1.6 millimeters. (Photos by August Jennewein)
For the last seven months, Kim Rankin had been on edge for a referral to Cincinnati Children’s Aerodigestive and Esophageal Center for her adopted son, Nathaniel.
She was finished waiting.
On a spring Saturday in 2015, Rankin bypassed normal channels and emailed the center’s director of research. She got an out-of-office reply. Then, a few hours later, an actual response: Nathaniel’s case was unusual. Someone would reach out.
At 8:05 a.m. the following Monday, Rankin received what turned out to be a life-changing call – a pivotal moment that represented a switch from uncertainty to stability.
About two years prior, Nathaniel was born with an airway of 1.6 millimeters, less than half the normal width for newborns, and rushed to the neonatal intensive care unit for an emergency surgery to implant a tracheostomy tube in his neck so he could breathe. The resulting trach was unstable: It needed to be tied in place and could be pulled out easily. With only 90 seconds to replace Nathaniel’s tube before he’d suffer from lack of oxygen, Rankin and her family could never let him be more than an arm’s length away.
Rankin – who’d earned a BA from the University of Missouri–St. Louis and was one year into an MA in English when she adopted Nathaniel – has used competencies gained at UMSL to inform his medical care, his education and outreach education. Throughout she’s been supported by community relationships and bonds with UMSL classmates and instructors – even contributing a testimonial to Associate Professor of English Suellynn Duffey’s forthcoming book.
Education and a dream
Rankin and her husband, Rich, already had the paperwork for a Missouri foster and adoption license sitting in their linen closet when they were recruited to adopt Nathaniel in 2013.
At the time, Rankin was one year into her UMSL master’s degree in English after earning her BA the previous year. A nontraditional student, she was wrapping up home-schooling her first batch of seven children and wanted to teach community college writing.
At UMSL, Rankin developed a synergistic relationship with her professors. She believes that attitude helped embolden her to reach out directly to Nathaniel’s surgeon.
“There were really open attitudes on the professors’ part to take my life experience and the curriculum and find connections there,” Rankin said. “There was almost a collaborative attitude versus a ‘you’re the teacher I’m the student’ hierarchy.
“I think I approached Nathaniel’s doctors – rather than looking at them like I had to do everything they said – like, no, we’re collaborating on this situation. I brought them information. They shared information with me. It was more like, ‘What do you think? Maybe we should try this? Maybe we should try that?’ Different things. My UMSL experience prepared me and influenced my willingness to say to the doctors, ‘No, I disagree.’”
When the Rankins saw photos of Nathaniel and heard his story – his biological mother passed away shortly after giving birth – they knew theirs was the family for him.
Diagnosed with subglottic stenosis and a laryngeal web, Nathaniel was born with webbing between his vocal cords, which remained frozen and prevented him from vocalizing, and narrowing that extended significantly down his trachea. His doctors didn’t expect him to live to his first birthday.
“That was very sad to me,” Rankin said. “He just needed a lot of love regardless of what the outcome was going to be. His time should be filled with love and happiness. I think we felt like we would continue to walk through open doors, and if it wasn’t supposed to happen, doors would close.”
Gaining stability
The first night Rankin brought Nathaniel home, he developed a mucus plug in his trach tube and couldn’t breathe. Their private nurse panicked and called 911. After a few tries, Rankin was able to change Nathaniel’s tube successfully herself, but the process taught her that many medical professionals did not know how to care for the unique needs of trach babies.
That experience led Rankin to Tricia Casey, a paramedic of the Rock Township Ambulance District. Casey was piloting a new program, the Special Needs Tracking and Awareness Response System, a database of individual dossiers on special needs children for first responders.
Rankin enrolled Nathaniel and drew on experience from UMSL and home schooling to participate in trainings for firehouses and ambulance districts.
“A couple Sundays we had multiple ambulances lined up out front,” she said. “We would teach them about emergency trach changes when we would do our routine trach changes. I think that willingness to have a teaching relationship with professionals whose worlds are very different from mine has probably contributed to changing community-based medicine in St. Louis.”
While Rankin and others were figuring out how to best care for Nathaniel, his medical situation seemed as fraught as ever. Routine changes distressed Nathaniel, and he’d periodically pull his tube out, which meant there always had to be two adults nearby.
Nathaniel was prone to illness and had four or five bouts of pneumonia per year. If he tried to eat orally, he’d start coughing and gagging and relied on gastronomy tube feedings. Rankin hoped Nathaniel would be a candidate for airway reconstruction so that he’d be able to speak vocally, but during the process of considering that surgery, doctors discovered fluid was getting into his lungs.
The pneumonia suddenly made sense. Widening his airway would make the aspiration worse, so he was not a candidate for reconstruction, but Rankin knew something had to change.
That eventually led her to Cincinnati Children’s Hospital, home to the only airway clinic in the United States. An interdisciplinary team of doctors recommended a laryngectomy, a surgery to remove Nathaniel’s larynx and separate his esophagus and trachea. He’d breathe through an opening in his neck known as a stoma, which would be more stable.
The procedure would also render Nathaniel completely mute. Rankin and her husband struggled but ultimately decided it was the right move.
“We’ve only had two bouts of pneumonia in the three years since surgery,” she said. “It really improved his quality of life and our quality of life, and also, the trach is much more secure. He’s pulled it out since surgery, and we were between two semitrucks on the highway. We had time to get over on the side of the road and put the tube back in whereas presurgery that potentially could have been a life-or-death situation.”
Writing, reading and speaking
Rankin writes extensively about AAC and home-schooling Nathaniel on her blog and Facebook page, Hold My Words.
Rankin dipped into her home-schooling and UMSL experiences to start Nathaniel’s education. Classes such as linguistics helped her work with the Saint Louis University speech language pathology department teaching Nathaniel how to form sounds with his mouth so that he may use an electrolarynx, a battery-powered external voice box.
Since starting that therapy, he’s begun making sounds with his mouth and learned to vocalize one word – mama.
Nathaniel also uses augmentative and alternative communication to speak. He signs and uses a voice generated output device, an app on an iPad with a special case, and is learning to make sentences.
Rankin writes extensively about AAC and home-schooling Nathaniel on her blog and Facebook page, Hold My Words. Started as a way to share information with friends and family, the two have become resources for others working through similar situations, speech language pathologists and educators.
Though she hopes to finish her master’s when Nathaniel is a bit older, Rankin no longer wishes to teach at a community college. However, education is clearly part of her future.
She’ll be the keynote speaker at an AAC conference later this year and is leading a breakout session as well.
“That conference will be attended by mostly school-based speech language pathologists, which is really interesting to me as a home-school mom,” she said. “I’ll be presenting to teachers and professionals who help kids in schools. It’s just kind of interesting how things worked out.”















